Urinary Tract Infections (UTIs) are a widespread issue that impacts countless individuals around the globe. Although they may appear simple at first glance, there’s a deeper complexity to UTIs that often goes unnoticed.
The purpose of this article is to present a thorough examination of UTIs, exploring their origins and the ramifications they entail.
An Overview
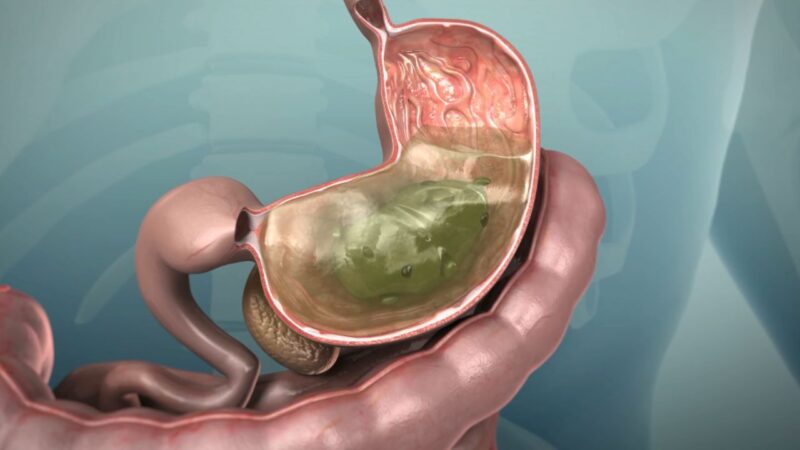
Urinary Tract Infections (UTIs) aren’t just one type of infection but rather a range of infections that can affect different parts of the urinary tract. They can show up in the urethra, bladder, and even the kidneys, taking on various forms, each with its own set of symptoms and complications.
To truly grasp how the urinary system works and how urine is created, it’s important to know about the mechanisms behind urine formation.
As per Anastasia Diakou, UTIs are infections that occur in the urinary tract. This includes infections in the urethra, known as urethritis, as well as infections in the bladder, known as cystitis. Infections in the kidneys are considered separately, falling under the category of acute pyelonephritis.
Etiology
It’s really important to grasp the underlying reasons behind UTIs if we want to prevent and treat them effectively. Although bacteria are the main culprits, the specific kinds of bacteria and the circumstances that promote their growth can differ.
When it comes to UTIs, bacteria are generally the ones to blame. There’s a whole range of organisms that can lead to an infection, but gram-negative bacteria tend to be the primary troublemakers. The majority of UTIs start with bacteria from the digestive system making their way into the urethra.
Anastasia Diakou’s research also states that bacterial biofilms play an important role in UTIs, being responsible for the persistence of infections that result in recurrence and relapse.
The most common organism responsible is Escherichia coli.
Other bacteria that can cause UTIs include:
- Proteus mirabilis
- Klebsiella pneumoniae
- Enterobacter
- Serratia
- Pseudomonas aeruginosa
Additionally, certain sexually transmitted diseases can also lead to UTIs, especially in young, sexually active individuals with recent new partners.
These organisms include:
- Chlamydia trachomatis
- Neisseria gonorrhea
- Ureaplasma urealyticum
Pathogenesis
The journey of bacteria through the urinary system is truly fascinating. It’s like they go on an adventure, starting from the urethra and potentially making their way to the kidneys. To really understand urinary tract infections (UTIs), it’s important to grasp this entire path.
Imagine the urinary tract and kidneys as a single continuous tube. So, when bacteria manage to get into the urethra and cause urethritis, they can easily extend their reach into the bladder, causing cystitis.
But it doesn’t stop there! Infections can actually travel upwards from the bladder through the ureters, and gain access to the kidneys through the renal pelvis and calyces. This progression leads to a more severe condition called acute pyelonephritis, which deserves its own discussion.
Clinical Consequences
When it comes to UTIs, the range of symptoms can vary from mild discomfort to severe pain and complications. It’s important to recognize these symptoms early on to ensure timely intervention and treatment.
For individuals at risk, the sudden onset of symptoms like painful urination, frequent and urgent need to urinate, and discomfort in the lower abdomen strongly suggest a UTI. In fact, the symptoms of cystitis and urethritis often overlap quite a bit.
Nevertheless, if you experience additional symptoms like general body discomfort and pain in the side, it’s likely that the infection has spread to the kidneys, indicating acute pyelonephritis.
Signs and Symptoms

While the clinical consequences provide a broad overview of UTI symptoms, it’s essential to dig deeper into the specific signs and symptoms that patients might experience.
Symptoms of uncomplicated UTIs are typically pain on urination (dysuria), frequent urination (frequency), inability to start the urine stream (hesitancy), sudden onset of the need to urinate (urgency), suprapubic pain or discomfort, bladder spasms, and blood in the urine (hematuria). – Michael J. Bono of Eastern Virginia Medical School
Complications
If left untreated, UTIs can lead to more severe complications. It’s essential to be aware of these potential outcomes to understand the importance of early detection and treatment.
As per Mariya Belyayeva, one of the primary complications of UTIs is the spread of the infection into the kidneys, known as acute pyelonephritis. This condition is more severe and requires immediate medical attention.
Risk Factors
Certain individuals are more susceptible to UTIs due to various risk factors. Recognizing these factors can help in prevention and early detection.
Several factors increase the likelihood of developing a UTI. These include female gender, sexual activity, pregnancy, urinary tract obstructions, the presence of renal and urinary tract stones, neurogenic bladder, diabetes mellitus, and the use of a Foley catheter.